When someone struggles with addiction, there’s often more hiding beneath the surface. Nearly half of individuals with substance use disorders also battle mental health conditions, yet most never receive integrated care. This article explores why dual diagnosis is more prevalent than many realize and how recognizing co-occurring disorders can transform recovery outcomes for adults, youth, and families seeking help.
Key Takeaways
- Dual diagnosis affects nearly half of people with substance use disorders, making it far more common than most realize
- Co-occurring psychotic, mood, and anxiety disorders frequently drive substance abuse as a form of self-medication
- Fragmented healthcare systems and inadequate screening allow many cases to go undiagnosed and untreated
- Integrated treatment addressing both mental health and addiction simultaneously produces significantly better outcomes
What Is Dual Diagnosis and Why Does It Matter?

Dual diagnosis in addiction treatment is when there is the simultaneous presence of mental illness and substance use disorders in one individual. Also called co-occurring disorders or concurrent disorders, this condition affects millions of American adults annually. When someone experiences both psychiatric disorders and addictive behaviors, each condition influences the other, creating a complex cycle that requires specialized treatment approaches.
Mental health disorders like major depressive disorder, bipolar disorder, anxiety disorders, and post-traumatic stress disorder frequently overlap with drug abuse and alcohol addiction. While the Diagnostic and Statistical Manual recognizes co-occurring disorders, some treatment programs aren’t properly equipped to handle them, leaving patients vulnerable to relapse and ongoing psychological distress.
The Staggering Prevalence of Co-Occurring Disorders
According to the Substance Abuse and Mental Health Services Administration, among people with severe mental illness, over 50% also struggle with substance abuse problems. At the same time, individuals seeking substance abuse treatment show mental health issues at much higher rates than the general population. Addressing substance abuse and mental health problems has become a widespread public health challenge affecting families across every demographic.
- Young adults face particularly elevated risk factors. Between ages 18 and 25, the brain continues developing while social pressures intensify, creating vulnerability to both psychiatric symptoms and drug use.
- Veterans returning from service, trauma survivors, and those with family histories of mental disorders or addiction face compounded risks for developing more than one disorder simultaneously.
- Individuals with chronic pain are another group that frequently struggles with co-occurring disorders, particularly the combination of substance use disorders and mental health conditions like depression and anxiety.
Why Dual Diagnosis Often Goes Unrecognized

Many people don’t realize they have co-occurring substance and mental health conditions because symptoms overlap considerably. Depression might drive someone to abuse alcohol as self-medication, while chronic drug abuse can trigger anxiety disorders or mood disorder symptoms. This chicken-and-egg scenario makes identifying the root cause incredibly challenging without a comprehensive assessment by mental health professionals.
The fragmented healthcare system in the United States compounds the problem. Traditional medical education often separates addiction treatment from psychiatric care, training specialists who may miss concurrent disorders outside their focus area. Insurance limitations, stigma, and inadequate screening protocols mean countless individuals receive partial treatment that addresses symptoms without tackling underlying psychiatric illness.
The Dangerous Cycle of Self-Medication
When psychiatric syndromes go untreated, many individuals unconsciously turn to substances for relief. This self-medication pattern provides momentary relief but ultimately worsens both conditions, creating negative consequences that spiral over time.
- Someone with social anxiety might discover that prescription medications or illicit drug use temporarily eases their discomfort in crowds.
- A person experiencing major depression may find that stimulants provide short-term energy boosts.
- Without intervention from a qualified treatment provider who recognizes this pattern, individuals become trapped in a cycle where each condition fuels the other, leading to deteriorating function, strained relationships, and increased risk of suicide attempts.
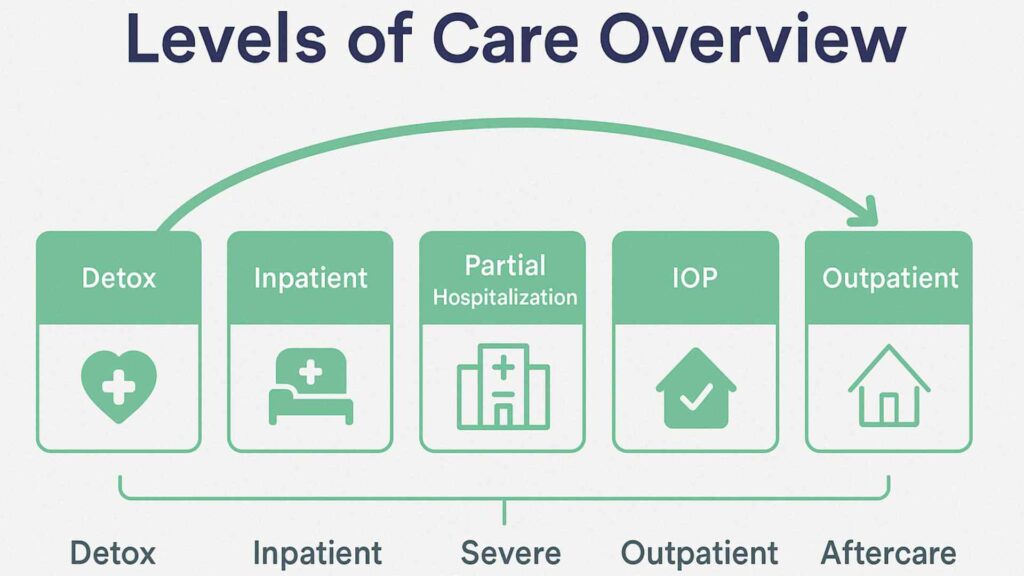
How Integrated Treatment Changes Everything
Treatment of dual diagnosis requires addressing both conditions simultaneously through the same treatment provider or coordinated treatment team. Behavioral therapy techniques like cognitive behavioral therapy help patients develop coping skills for managing psychiatric symptoms without turning to substances. Psychiatric medication may stabilize mood disorders or anxiety disorders, reducing the urge to self-medicate.
Dual diagnosis programs incorporate support groups, talk therapy, family education, and medical monitoring for withdrawal symptoms. This integrated treatment approach recognizes that lasting recovery requires healing the whole person. Studies show patients receiving concurrent treatment for both their mental health and substance issues achieve better outcomes than those treated for conditions separately, with lower relapse rates and improved quality of life.
Dual Diagnosis Frequently Asked Questions
What is the best treatment for dual diagnosis?
Integrated treatment addressing both mental health and substance use disorders simultaneously is most effective. This typically combines evidence-based psychotherapy (like CBT or DBT), medication management, peer support groups, and coordinated care from specialists trained in treating co-occurring conditions together rather than separately.
What medication is used for dual diagnosis?
Medication depends on specific diagnoses. Common options include antidepressants (SSRIs, SNRIs), mood stabilizers (lithium, valproate), antipsychotics (risperidone, olanzapine), and medications for substance use disorders (naltrexone, buprenorphine, acamprosate). Treatment plans are individualized based on each person’s unique combination of conditions.
Find Hope Through Dual Diagnosis Care
Struggling with both addiction and mental health challenges? You don’t have to face them alone. At Abundance Treatment in Toledo, our dual diagnosis support addresses substance use and co-occurring conditions together through structured PHP, IOP, and outpatient programs. We treat you like family in a welcoming, judgment-free environment. Take the first step toward your abundant life, reach out to us today.