An intensive outpatient program, often called IOP, plays a key role in recovery for people who need clinical care without living at a facility full-time. Many people considering this level of care want one clear answer first: how long does this type of program last?
This article explains typical timelines, factors that affect program length, how progress is measured, and how intensive outpatient care fits into the recovery spectrum.

What an Intensive Outpatient Program Is Designed to Do
An intensive outpatient program provides scheduled treatment while allowing participants to live at home. It offers frequent therapy sessions, education, and recovery planning while allowing individuals to fulfill daily responsibilities, such as work, school, or family duties.
IOP focuses on overcoming substance abuse, addressing behavioral drivers of use, and reinforcing coping skills. Sessions often include group therapy, individual counseling, relapse prevention education, and mental health screening. Medical oversight may also be part of the treatment when appropriate. The goal is to build stability without requiring residential placement.
Typical Length of an IOP for Substance Abuse
Most intensive outpatient programs last between eight and twelve weeks. This timeframe provides enough clinical contact to reinforce behavioral patterns and reduce relapse risk while still allowing flexibility for daily responsibilities. Shorter timeframes, often four to six weeks, may be appropriate when stability is already present and clinical needs are lower.
Extended treatment may reach sixteen weeks or longer when symptoms remain active or when co-occurring mental health concerns require continued focus. Duration is not set at enrollment. Length is adjusted based on attendance patterns, symptom control, and demonstrated readiness to stop abusing substances.
Rather than targeting a fixed end date, time in IOPs is guided by clinical indicators. Craving intensity, stress response, decision-making patterns, and consistent use of coping skills help determine how long this level of care remains appropriate.
Weekly Time Commitment and Program Intensity
While total program length is measured in weeks, intensity is measured in hours per week. Most IOPs require nine to fifteen hours of scheduled treatment each week. This often breaks down into three to five sessions spread across weekdays or evenings.
Early weeks tend to involve higher frequency sessions to stabilize routines and address immediate risks. As progress strengthens, session frequency may decrease while skills practice increases outside of therapy. This gradual shift helps prepare participants for step-down care.
The weekly schedule matters as much as the total length. Regular engagement reinforces habits, supports accountability through peer interaction, and strengthens coping responses under real-world pressure.
Factors That Influence How Long IOP Lasts
Substance use history is a primary determinant. Long-term polysubstance dependence or severe withdrawal risks demand prolonged phases to address cravings, rebuild neural pathways, and prevent relapse. Shorter histories allow faster progression.
Co-occurring mental health conditions like depression, anxiety, PTSD, or bipolar disorder complicate treatment. These necessitate integrated dual-diagnosis care that extends IOP to manage intertwined symptoms and reduce dropout rates. Home and social environment stability play a critical role.
Supportive family networks and trigger-free living accelerate completion. Unstable housing, toxic relationships, or easy access to substances prolong participation.
Patient engagement levels directly impact timelines. Consistent attendance, active therapy participation, homework adherence, and real-world skill application signal readiness for step-down care. Poor motivation, missed sessions, or repeated relapses justify extensions for safety and efficacy.
External factors such as employment demands, legal obligations, insurance coverage, and program-specific milestones (e.g., negative drug tests or therapeutic goals) further tailor duration. This ensures personalized paths that prioritize long-term recovery over rigid schedules.

How Progress Is Evaluated During an IOP
Regular urine drug screens and breathalyzer tests serve as primary biomarkers, confirming abstinence from target substances and detecting any use of alcohol or other drugs, with consistent negative results indicating physiological stability.
Attendance and participation metrics are closely monitored, including session compliance, completion of assigned homework, and engagement in group therapy, individual counseling, or family sessions, where active involvement signals motivation and skill acquisition.
Psychosocial assessments, such as standardized scales for depression, anxiety, or craving intensity, quantify improvements in mental health and daily functioning. At the same time, self-reported journals or relapse prevention plans reveal real-world application of coping strategies.
Therapeutic progress is further gauged by milestone achievements, like developing a sober support network, securing employment or housing, or demonstrating emotional regulation during role-playing exercises.
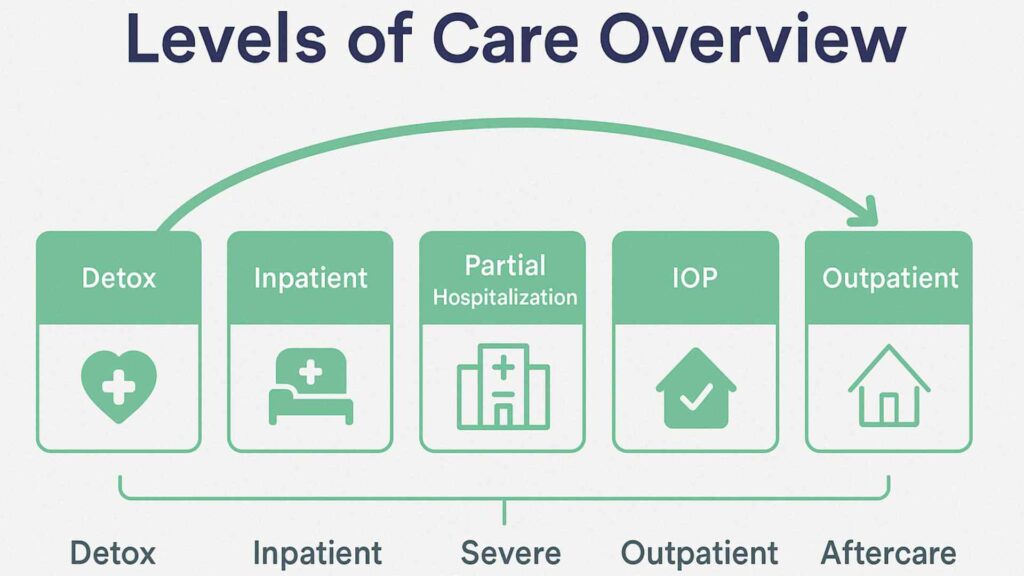
What Happens After an Intensive Outpatient Program Ends
Finishing an intensive outpatient program does not mean clinical care stops. Most people move into standard outpatient therapy, less frequent counseling sessions, or peer-based support groups that meet weekly or biweekly. This step-down approach preserves clinical oversight while gradually reducing treatment hours.
Aftercare often includes scheduled counseling sessions, ongoing peer support, and a clearly defined relapse prevention plan that identifies triggers, warning signs, and response strategies. These components reinforce progress made during IOP and help maintain stability as the external structure decreases.
Outcomes improve when intensive outpatient services are used as part of a broader treatment plan rather than as a single endpoint.
Also, you can take a look at our Alumni Rehab Program, where you can stay connected with a supportive community, reinforce positive habits, and keep progressing toward your goals.
Final Thoughts from Abundance Treatment
An intensive outpatient program usually lasts eight to twelve weeks, though the length varies based on symptoms, engagement, and clinical needs. The most effective IOP timelines respond to progress rather than calendar dates, allowing treatment to match recovery readiness.
At Abundance Treatment, we focus on measurable progress, practical skill development, and long-term stability. Our intensive outpatient treatment program in Toledo, OH, carefully evaluates progress through real outcomes, such as consistent sobriety, engagement, and skill application, then adjusts care duration accordingly, helping each person move forward with confidence and support rooted in evidence-based practice.