Alcohol misuse can affect the brain in ways that go beyond memory loss, poor judgment, or short-term confusion. One concern that often raises questions is whether alcohol misuse can lead to psychosis. Understanding how this develops helps people recognize early warning signs and seek timely support.
This article explains how heavy drinking impacts the brain, what psychotic symptoms may look like, why these reactions occur, and how treatment can reduce risks for long-term harm.

What Is Alcohol-Induced Psychosis?
Alcohol-induced psychosis refers to hallucinations, delusions, or severe confusion triggered directly by heavy drinking or sudden withdrawal. These symptoms resemble other psychiatric disorders, though the cause is tied to the impact of long-term drinking on the brain. This condition often appears during extended periods of misuse or when use stops abruptly after dependence has formed.
Heavy drinking affects neurotransmitters involved in mood, perception, and cognition. When levels of alcohol rise and fall, the brain struggles to regulate these systems, creating abnormal sensory experiences. This form of psychosis can be temporary, though it is still a medical emergency that requires quick intervention. Leaving symptoms untreated increases the risk of injury, relapse, or long-term mental health concerns, making timely enrollment in an alcohol rehab an important part of helping someone regain clearer thinking and safer functioning.
How Alcohol Misuse Leads to Psychosis
Alcohol disrupts multiple areas of the brain that stabilize perception and judgment. Heavy drinking strains these pathways to the point where the person cannot function normally, especially once dependence sets in. Several factors explain why psychosis can emerge.
One cause involves changes in the brain’s dopamine system. Dopamine influences reward, motivation, and interpretation of reality. Heavy use spikes dopamine levels, and repeated misuse pushes this system into dysregulation, which can create delusional thinking or unusual sensory experiences. Another factor is the pressure long-term drinking places on the GABA and glutamate systems. These regulate the balance between calming and excitatory signals in the brain. When tolerance forms, the brain demands more substance exposure to stay balanced. Once the substance’s levels drop, brain activity becomes erratic, which can trigger hallucinations or paranoia.
Nutritional deficiencies also play a significant role, as long-term misuse often leads to low levels of thiamine, folate, and other nutrients essential for healthy brain function. Severe thiamine deficiency can progress into Wernicke–Korsakoff syndrome, a condition that includes confusion, memory loss, and disturbed perception. These neurological changes increase vulnerability to psychosis, especially when drinking is chronic.
Types of Alcohol-Related Psychosis
- Alcohol Hallucinosis: This condition involves hearing, seeing, or feeling things that are not present. These hallucinations often begin within a day of stopping use and can last for several days. Individuals may remain aware of their surroundings but still struggle to separate hallucinations from reality.
- Alcohol Withdrawal Delirium (Delirium Tremens): This is the most severe form of withdrawal-related psychosis. Symptoms include extreme confusion, shaking, rapid heart rate, fever, and vivid hallucinations. Delirium tremens can be life-threatening and needs medical care right away.
- Chronic Alcohol-Induced Psychotic Disorder: Psychosis continues beyond the withdrawal phase. This long-lasting form resembles schizophrenia but is linked to extended misuse. It often requires ongoing psychiatric support due to the depth of cognitive and perceptual changes involved.
Each type presents a serious health risk, and anyone showing these symptoms needs medical attention immediately, even if they have not completely stopped drinking. Early intervention, detoxification, and treatment reduce complications and support long-term recovery.

Common Signs and Symptoms
Hallucinations are among the most recognizable signs and can be auditory, visual, or tactile. Some individuals hear voices, while others see shadows, shapes, or figures that are not real. Delusions are another sign, such as strong beliefs that others are watching, threatening, or judging them. These thoughts feel convincing, even when there is no evidence.
Confusion, agitation, disorganized thinking, and intense fear often appear alongside hallucinations or delusions. Some individuals have trouble understanding where they are or what is happening. Sleep disturbances, irritability, tremors, and rapid changes in mood may also emerge. When symptoms occur during withdrawal, physical signs like sweating, high blood pressure, or shaking may accompany psychological distress. These symptoms should always be treated as urgent, as they can worsen quickly, and delaying care increases the risk of harmful behaviors, irrational decisions, accidents, or relapse.
Treatment for Alcohol-Induced Psychosis
Alcohol-related psychosis requires immediate medical support, and the priority is stabilizing the individual in a safe environment. Medical teams monitor vital signs, correct dehydration, and address nutrient deficiencies, especially thiamine. Medications like benzodiazepines and antipsychotics may be used to reduce hallucinations, calm agitation, and ease withdrawal.
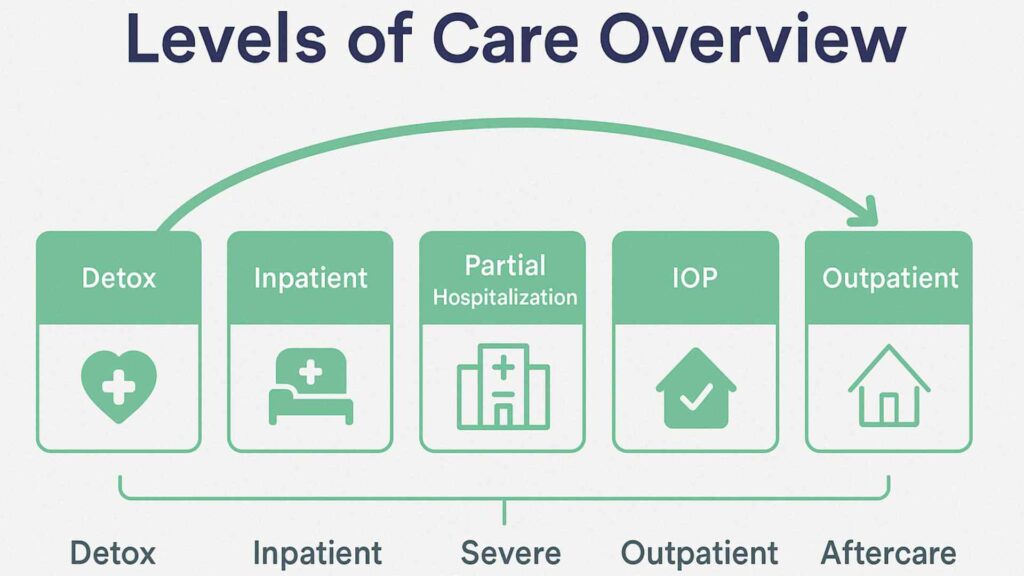
Once symptoms stabilize, long-term care focuses on treating AUD through inpatient or outpatient treatment programs that match the level of care the person needs. This often includes counseling, behavioral therapies, and support programs that address triggers, cravings, and co-occurring mental health symptoms. Addressing both psychosis and addiction creates a stronger foundation for recovery.
Medical professionals may also recommend ongoing psychiatric care if psychotic symptoms persist. This is common when heavy drinking has caused lasting neurological changes. Continued therapy helps individuals manage stress, strengthen coping skills, and rebuild daily stability. Support from family and friends, along with a recovery-focused environment, improves long-term outcomes.
Final Thoughts from Abundance Treatment
Alcohol misuse can create serious disruptions in the brain, and psychosis is one of the most concerning outcomes. Understanding how these symptoms develop gives individuals and families a clearer sense of when to seek help and what treatment involves. Quick action gives people the best chance to recover safely.
At Abundance Treatment, we help individuals experiencing alcohol-related symptoms and mental health concerns through targeted, clinically grounded care. Our alcohol addiction program in Toledo, OH, centers on treatment and stabilization, explores the underlying factors driving misuse, and guides clients toward long-term recovery with evidence-based treatment.